The SDoH literature use terms such as "health inequities" and "health disparities" to describe different population health outcomes. What is the critical distinction between these concepts.
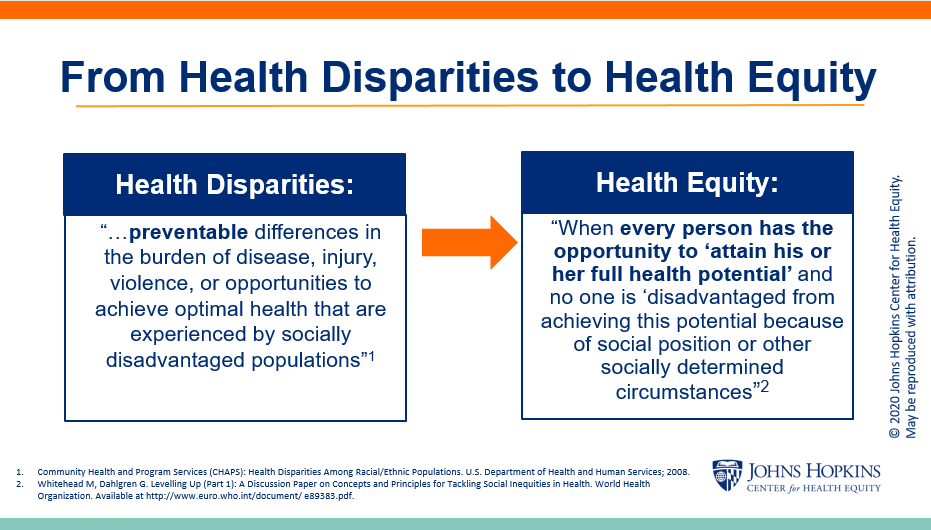
Health inequities- This is defined as an unfair avoidable advantage in healthcare whereby a group of people or community are better off than another. 
Health Disparities- measurable differences in health status that can be measured base on this can include but not limited to “ race and ethnicity, gender, employment and socioeconomic status, disability and immigration status, geography” (Sciences et al., 2017).

Health disparities- systemic disadvantage that is measurable
Health inequities- systemic advantage that is avoidable
What explains the lack of progress toward reducing health disparities among vulnerable groups?
Racism, discrimination, education, income and wealth, health systems and the services they provide, transportation, housing, Employment, to name a few.
Education-
Education is very vital when it comes to health disparities among vulnerable groups. There are extensive research that has shown correlation between a person educational level and their health status (Weinstein et al.). A study published in the Annu Rev Public Health found that, the highly educated are living longer compared to less educated people (Zajacova & Lawrence, 2018). It is not a secret that most health care professional’s knows, highly educated people are able to make better health decision. Educated individuals are able to read health information and comprehend it better. During my career as a nurse, I have utilized the teach-back method’s to make sure my patients have understanding to what is require of them after discharge.
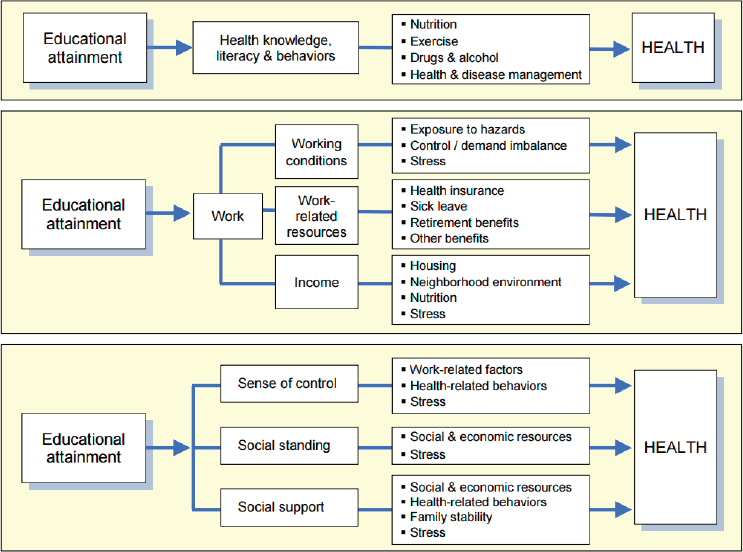
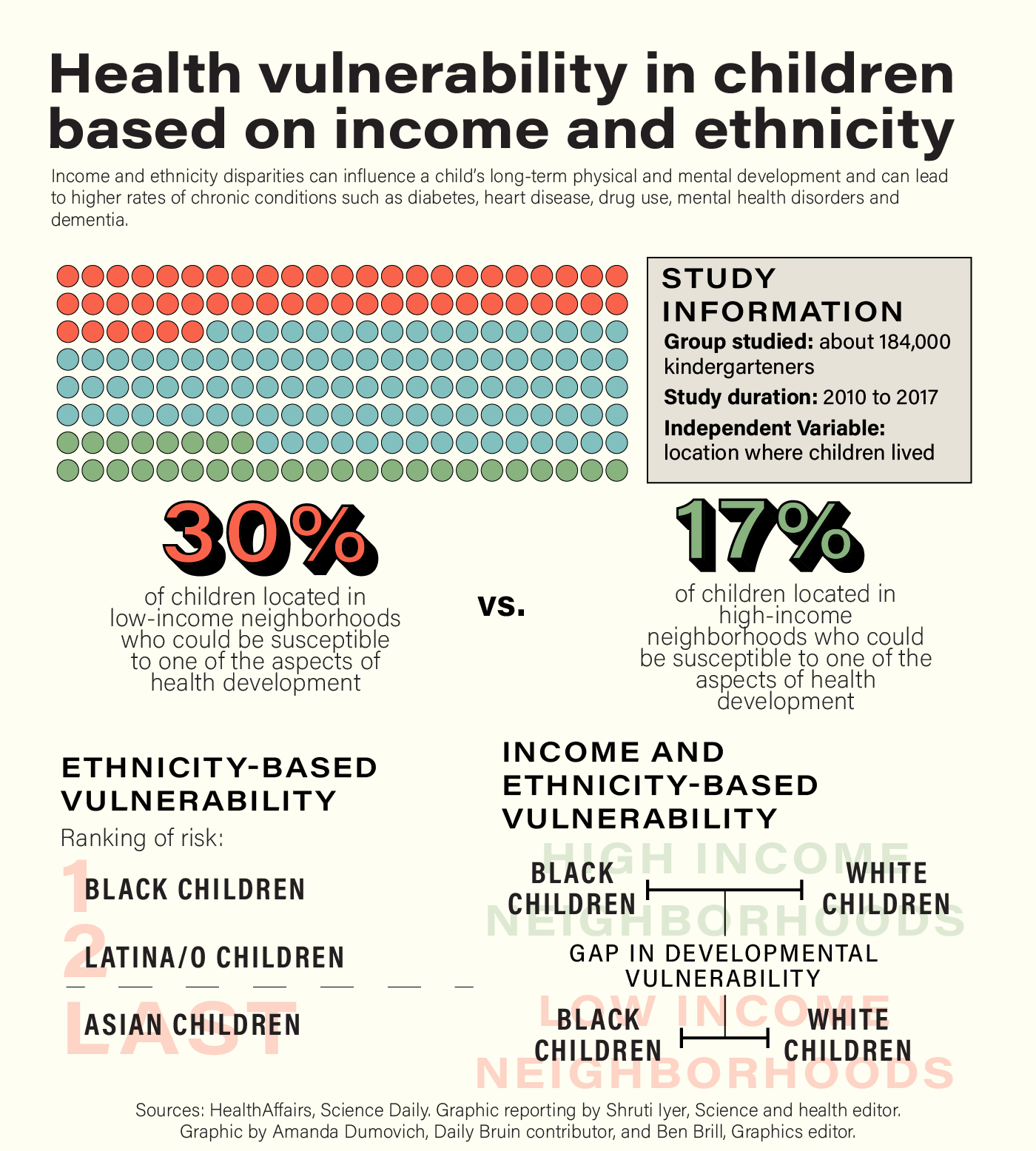
Income-Wealth-Employment-
Growing up, I heard the phrase money talk’s over and over again. Income, Wealth and Employment status has been found to be a predictor of health outcomes. People who are wealthy are able to afford better treatment. Chronic disease has been showed to be more among low-income people (Weinstein et al.). Whom your employer, is gives you access to a health network that you can afford. Most companies have some form of health insurance, employees can choose they leave of care their employer should cover by selection a health plan. Growing up in an inner city, my high schools was classified as low income. “National Equity Atlas data reveal that in about half of the largest 100 cities in the United States, most African American and Hispanic students attend schools where at least 75 percent of all students qualify as poor or low-income under federal guidelines” (Boschma, 2016).
Healthy systems-
Healthy systems- Health care includes but not limited to “preventative care, chronic disease management, emergency services, mental health services, dental care, and, more recently, the promotion of community services and conditions that promote health over the lifespan” (Weinstein et al.). Census block group (CBG) did a consumer study found black neighborhoods had higher access to fast-foods. Fast-foods for years has been known to have an influence on health and obesity risk (2016). All forms of healthcare is good and black neighborhoods should have access to healthy grocery stores, urgent cares and other preventative care channels instead of fast-food market's.
Transportation/ Housing
Homelessness not having a roof over once head and lack of transportation to seek health treatment is another was health disparities is still in active in healthcare. When you live next to a park, it is very likely that you may take your family to the park. It been found that access to green space has been showed to reduce stress, can improve mental health, and reduce mortality rate (Weinstein et al.). Working in healthcare, there are always people who miss their appointment because they didn’t have a ride.
Racism and Discrimination-
“Racism is not an attribute of minority groups; rather, it is an aspect of the social context and is linked with the differential power relations among racial and ethnic groups” (Weinstein et al.). Even though most study on racism in healthcare focus on minorities, every individual can experience racism or discrimination.
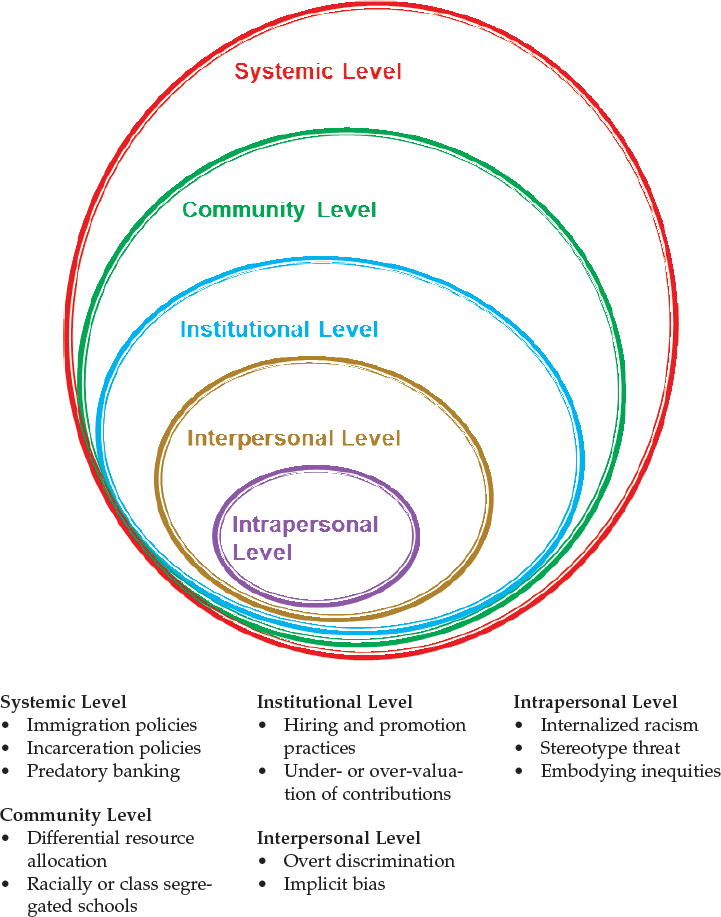
Should the SDoH be the responsibility of health professionals?
“Social determinants of health (SDOH) are the conditions in the environments where people are born, live, learn, work, play, worship, and age that affect a wide range of health, functioning, and quality-of-life outcomes and risks” (Healthy People 2030). This shouldn’t be the responsibility of a health professional. Health professionals can only solve structural inequities like racism, sexism, homophobia, classism when treating their patient’s (Weinstein et al.). Where a person lives, worship, and most of SDOH has nothing to do with health professionals.

In what ways has COVID-19 impacted by the social determinants of health?
The COVID pandemic has intensified health risk to the homeless population. In a Boston study of 408 individuals residing in a shelter, 147 (36%) had a positive SARS-CoV-2 PCR test (Abrams & Szefler, 2020). There has been an increase in private wealth, whiles the average worker has had a decrease in social wages (Paremoer et al., 2021). Study found "being younger, female, lower in education, having a previous psychiatric diagnosis lead to overeating during the COVID-19 pandemic: Lower income, being non-white, having a high-risk medical condition, higher BMI, experiencing negative mental health did very little physical activities during the lockdowns" (Robinson et al., 2021).
Olayiwola, N. (2020, December 7). Combating racism and place-ism in Medicine | J. Nwando Olayiwola | tedxkinglincolnbronzeville. YouTube. Retrieved September 19, 2021, from https://www.youtube.com/watch?v=0bnm__UPTRM.
A, N. (2019, February). Homelessness & Health: What’s the Connection? National Health Care for the Homeless Council. Retrieved September 18, 2021, from https://nhchc.org/wp-content/uploads/2019/08/homelessness-and-health.pdf.
A, N. (2021). Social Determinants of Health. Social Determinants of Health - Healthy People 2030. Retrieved September 19, 2021, from https://health.gov/healthypeople/objectives-and-data/social-determinants-health.
A, N. (2021, February 10). Even Albert knew this –the turning point of health care calls for completely new kind of thinking. Movendos. Retrieved September 19, 2021, from https://movendos.com/en/even-albert-knew-this-the-turning-point-of-healthcare-calls-for-completely-new-kind-of-thinking/.
Abrams, E. M., & Szefler, S. J. (2020, July). Covid-19 and the impact of Social Determinants of Health. The Lancet. Respiratory medicine. Retrieved September 19, 2021, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7234789/.
James, P., Arcaya, M. C., Parker, D. M., Tucker-Seeley, R. D., & Subramanian, S. V. (2014, September). Do minority and poor neighborhoods have higher access to fast-food restaurants in the United States? Health & place. Retrieved September 18, 2021, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4783380/.
Paremoer, L., Nandi, S., Serag, H., & Baum, F. (2021, January 29). Covid-19 pandemic and the Social Determinants of Health. The BMJ. Retrieved September 19, 2021, from https://www.bmj.com/content/372/bmj.n129.
Robinson, E., Boyland, E., Chisholm, A., Harrold, J., Maloney, N. G., Marty, L., Mead, B. R., Noonan, R., & Hardman, C. A. (2021, January 1). Obesity, eating behavior and physical activity during COVID-19 lockdown: A study of UK adults. Appetite. Retrieved September 19, 2021, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7540284/.
Sciences, N. A. of, Engineering, & Medicine, and. (2017, January 11). The root causes of health inequity. Communities in Action: Pathways to Health Equity. Retrieved September 16, 2021, from https://www.ncbi.nlm.nih.gov/books/NBK425845/.
Shruti Iyer. (2020, October 30). UCLA researchers find health care inequalities adversely affect low-income youth. Daily Bruin. Retrieved September 18, 2021, from https://dailybruin.com/2020/10/30/ucla-researchers-find-health-care-inequalities-adversely-affect-low-income-youth.
Weinstein, J. N., Baciu, A., Negussie, Y., & Geller, A. (n.d.). Read "Communities in action: Pathways to health equity" at nap.edu. National Academies Press: OpenBook. Retrieved September 18, 2021, from https://www.nap.edu/read/24624/chapter/5#120.
Zajacova, A., & Lawrence, E. M. (2018, April 1). The relationship between education and health: Reducing disparities through a contextual approach. Annual review of public health. Retrieved September 18, 2021, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5880718/.

Comments
Post a Comment